
Multidisciplinary Clinic of Metabolic & Bariatric Surgery

 Obesity Surgery - Obesity Surgery -
 Management Team Management Team

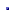 Minimally Invasive Minimally Invasive
 Bariatric Procedure Bariatric Procedure

|
Combine Obesity Clinic
CUHK Combined Obesity Clinic (COC) in the Prince of Wales Hospital is University-based clinic which heavily
subsidized by Surgical Department of CUHK. COC is a multi-disciplinary clinic, which recruit the input of
involved surgeons, endocrinologists, dietitians and specialty nurses to provide assessment and counseling on
those patients with severe obesity who need bariatric intervention. It provided preoperative counseling,
endocrine and metabolic disease screening for secondary causes of obesity and obesity-associated co-morbidities,
dietary assessment and counseling and if required, psychiatric assessment for the morbidly obese patients
before bariatric procedure is contemplated. Apart from clinical service, COC also provide platform in clinical
researches related to epidemiology and management of obesity.
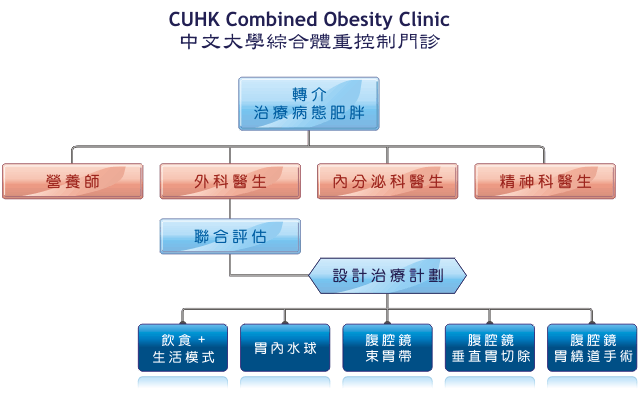
OBESITY SURGERY - MANAGEMENT TEAM
Morbid obesity is a multi-factorial disease which involves elements of heredity, biochemistry, hormones,
environment, behavior, and culture. Therefore, the management of obesity is a multidisciplinary task
involving not only the skills of the bariatric surgeon, but also those of other healthcare professionals.
 |
Obesity Surgeons

Bariatric Surgeon plays a leading role in obesity surgery management team. Starting from preoperative
management with assessment and education and counseling , followed by performing the procedure and peri-operative
care and together with post-operative follow-up and detection of potential complications, the surgical team always
act as the leader of the team & guidance of our patients.
|
 |
Dietician

Patient compliance with required dietary modifications obesity surgery is a key factor in determining outcome. Thus,
nutritional education, management and supervision are essential elements in the patient’s success and the dieticianis a vital part of the team.
|
 |
Anesthesiologist

Surgery in the morbidly obese is a potentially high-risk procedure as there are pathophysiological changes induced
by morbid obesity that complicate patient management during anesthesia. Therefore, the anesthesiologist must be
thoroughly familiar with the obese patient, the procedure and all possible complications; both intra-operatively
and post-operatively.
|
 |
Internist, Gastroenterologist, Endocrinologist

The major function of endoscopy prior to obesity surgery is to detect the presence of anatomical particularities
and pathologies of the upper GI tract since some pathologies may delay or even contraindicate the procedure.
Endoscopy is also important post-operatively for identification of certain complications. The role of endocrinologist
& internist is to identify and optimize the obesity related medical diseases and the appropriate adjustment of
medication & treatment after successful weight reduction surgery.
|
 |
Specialty Nurse

Nurses are frequently the front line of contact with the patient. They provide explanations, education, reinforcement,
praise, recognition, comfort, trouble-shooting, and advocacy for the patient, all toward the goal of improved health.
Some of the ultimate nurse’s goals for the treatment of the obese patient are weight loss, enhanced self-esteem and
improved quality of life.
|
 |
Psychiatrist

The roles of obesity surgery and psychological surroundings are interrelated. Pre-operative psychological testing
is required in order to determine personality structure and behavior, detect any psychological contraindications
and to reveal the importance of post-operative psychological follow-up. It is also important to rule out major
psychiatric disorder and substance abuse before considering obesity surgery.
|
 |
Physiotherapist

Continuity of physical exercise can be a very important in determining long-term success for the patient after
obesity surgery. However, it is sometimes difficult for patients to discipline themselves on a regular basis and
the physiotherapist is necessary to lend support by creating exercise programs and giving patients tools by which
they can help themselves.
|
 |
Radiologist

Specialty knowledge on operative procedure and possible post-operative problem allows early detection of
post-operative progress. Post-operative imaging of various bariatric procedure is essential in subsequent
management of patient after they received surgery.
|
MINIMAL INVASIVE APPROACH IN BARIATRIC SURGERY
Surgeries for morbidly obese patients are technical challenging. Traditional open surgery requires a long
incision which can lead to wound healing problem. The pain that induced by big wound can also lead to a list
of post-operative complication secondary to immobilization, such as chest infection and blood clots formation
in leg veins. Minimal invasive approach largely reduced the above problems and speed up the recovery after surgery.
Minimally invasive approach now includes Laparoscopic surgery and Endoscopic procedures.
What Is Laparoscopic Surgery?
Laparoscopic surgery is a new surgical specialty which involves operating through small incisions, using a long
slender camera and lens system to view the internal organs. It requires general anesthesia with 5 to 6 small
incision are made on your tummy so that surgeons can operate inside the abdomen with special laparoscopic instruments
without a large incision.
Laparoscopic Surgery

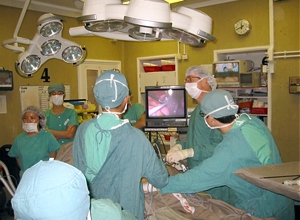
|
 |
Key hole scar after surgery

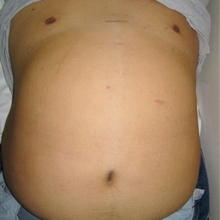
|
What is Endoscopic Procedure?
Endoscopy is a minimally-invasive medical procedure in which a flexible tube is used to inserted through the mouth and
down into the stomach to examine and performing therapy. Endoscopic procedure does not require skin incision and all
procedures are performed under sedation.
Endoscopic Procedure

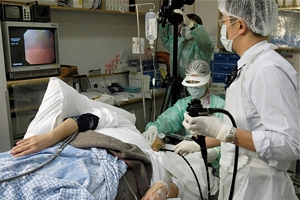

|





